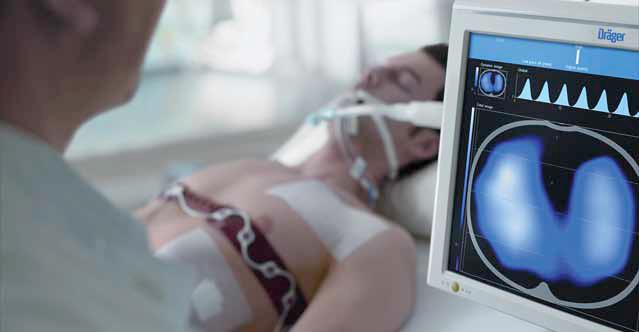
The new PulmoVista 500 is the first EIT device (Electrical Impedance Tomography) intended for everyday clinical use by intensivists to view regional distribution of lung ventilation directly at the bedside. With up to 50 images per second, physicians can track the effects of intensive care ventilation in real time
Nikil Rao
General Manager,
Draeger Medical India Pvt Limited
The University Hospital Leipzig is the first hospital in the world to implement the PulmoVista 500. Mechanical ventilation uses pressures that are much higher than normal breathing which creates a risk of overstretching areas of the lung. On the other hand, if the pressure at the end of the breath is set too low, some lung areas may collapse. Both of these situations can impede the healing process of an intensive care patient. Upto now, Computed Tomography (CT) has given the physician a clear picture of the status of the lung, albeit only as a snapshot in time. PulmoVista 500 now delivers complementary information in the form of dynamic images “ comparable to a film sequence. The physician can continuously track how the breathing gas volume generated by the ventilator is distributed in the lungs. With EIT, we can now see how ventilation of the lung changes and subsequently functionally uate the changes. This is the first time this type of assessment has been made available, said Prof Dr Hermann Wrigge, Deputy Director of the Clinic and Polyclinic for Anaesthesiology and Intensive Care at the University Hospital Leipzig, the first hospital in the world to use EIT device from Dr¤ger. Measurements are performed using a flexible belt, with 16 integrated elec trodes, placed around the patients chest. The electrodes apply a small current to the patients body; the resulting voltages change according to the amount of air in the lungs. PulmoVista 500 uses the measured voltages to create tomographic images of the lung function.
An important step in lung protective ventilation
PulmoVista 500 supports therapy management by continuously updating images of regional distribution of ventilation. For example, if the physician changes the PEEP (positive end-expiratory pressure) on the ventilator, the EIT device immediately shows the effects on the distribution of the ventilation and end-expiratory lung volume. The PEEP, the airway pressure at the end of a breath, must not be set too low in order to prevent the alveoli from collapsing. On the other hand, if the PEEP is set too high this may result in areas of the lung being overstretched which may damage the lung. Studies show that EIT can continuously provide information about the recruitability of the lungs and elecoptimal
PEEP settings. This feature can help users optimise distribution of ventilation in the lung. Prof Dr Christian Putensen, Head of Surgical Intensive Care at University Hospital Bonn, has conducted research about clinical applications of EIT since 2003. Further underscoring the use of EIT to guide mechanical ventilation, he stated: EIT support for setting ventilation parameters clearly has the potential to improve gas exchange for patients with respiratory complications.
One of the primary goals in developing PulmoVista 500 was to make sure that the device was easy to use in the demanding intensive care environment: Thanks to the easy to attach flexible electrode belt the device is ready for use in just a few minutes. Measured values as well as previously recorded EIT data can both be accessed at the bedside. Furthermore, because the noninvasive EIT procedure can be completed without radiation PulmoVista 500 supports ventilation monitoring without side effects.
Be a part of Elets Collaborative Initiatives. Join Us for Upcoming Events and explore business opportunities. Like us on Facebook , connect with us on LinkedIn and follow us on Twitter , Instagram.
"Exciting news! Elets technomedia is now on WhatsApp Channels Subscribe today by clicking the link and stay updated with the latest insights!" Click here!