As the world is reeling under Corona crisis and various administrations trying to find ways to deal with the highly contagious virus, testing seems to be the only way to take stock of the exact situation — Unlike other virus the SARS-CoV-2 is little tricky as half the symptomatic patients who tested negative for Covid-19 in an are detected positive in two-three weeks.
As per experts the virus needs to be tackled in a planned and strategic manner and testing plays a huge significance at this juncture. As the COVID positive cases touch a million, everyday more people get affected more tests rapid antigen testing is done to contain the viral infection leading to lesser number of mortality.
According to the World Health Organisation (WHO) the official figure, the cumulative number of samples tested, as of now is 1,24,12,664. 22 States/UTs in India are already conducting 140 and more tests per day per million.
Also read: ‘India’s covid-19 fatality rate one of the lowest globally’
The union health ministry and Indian Council of Medical Research (ICMR) have repeatedly urged states to follow the ‘Test-Track-Treat’ strategy for early detection and containment of the outbreak. Understanding the need to test more numbers of samples to break the cycle of the infection. Centre and state government are working unanimously to scale up the testing infrastructure.
Rapid Antigen Test provides quick results
Even though RT-PCR (reverse transcription-polymerase chain reaction) remains the gold standard of frontline testing for the novel coronavirus, there has been a range of tests including Antigen, Antibody, TrueNat and CBNAAT tests (tuberculosis tests).
Currently, the majority of the tests being conducted in India and worldwide are RT-PCR which takes around 5-6 hours to give results. Antibody test, also called serology test, used to estimate population exposed to infection/ and for survey in high-risk groups. Rapid Antigen Testing is being considered the best way to get quick results–it takes 30 minutes.
The major drawback of this test is its accuracy, many who test negative in these tests might have to go for a confirmatory RT-PCR test. After a strong appeal by the Centre and ICMR, ten high case-load states and a union territory recently decided to introduce rapid antigen tests which give “highly specific” results in 30 minutes.
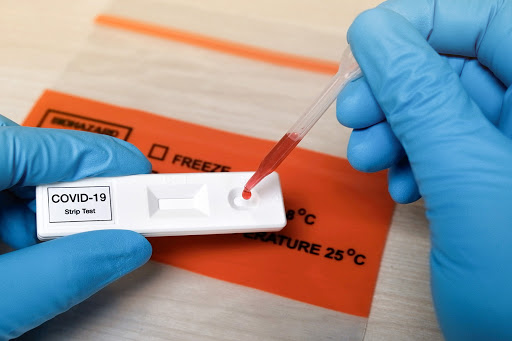
The Delhi government is already using the antigen testing to detect infection in asymptomatic persons. Other states like Maharashtra, Gujarat, Karnataka, Kerala, Punjab, Haryana, where case loads are high, have decided to deploy antigen kits to detect infection in a quick possible manner.
Antigen vs antibody
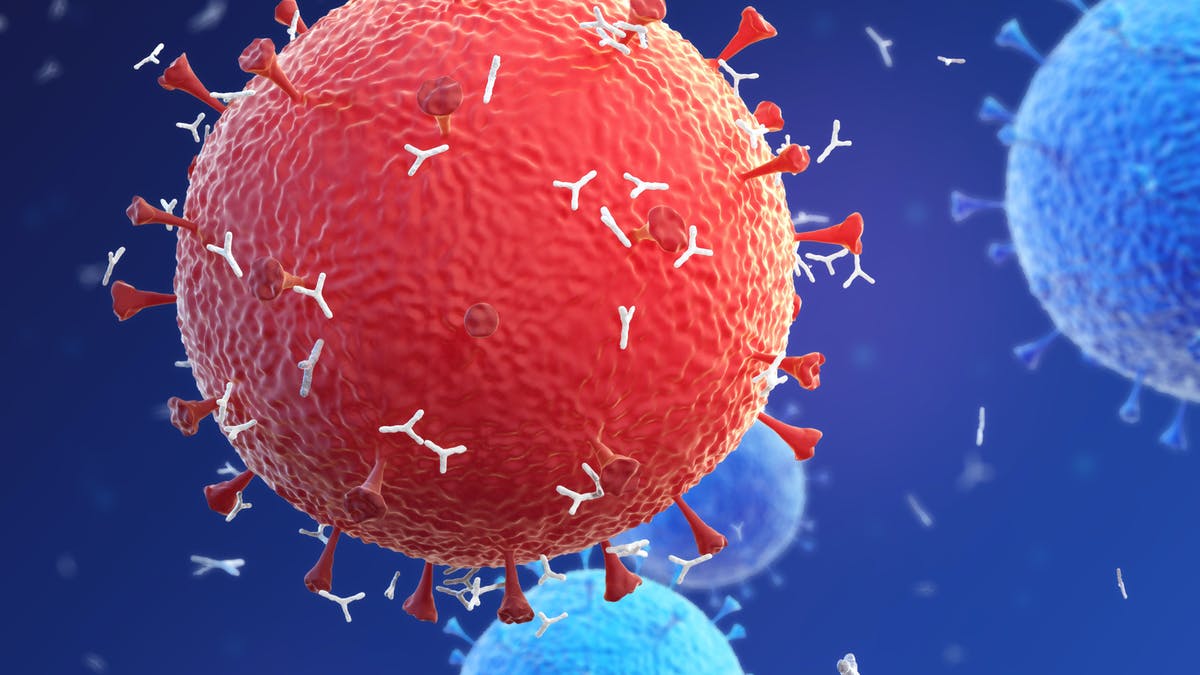
In order to know how antigen testing works, one should know the biology of Antigen and antibody in brief. An antigen is a molecule capable of stimulating an immune response. They may be proteins, polysaccharides, lipids or nucleic acids. Each antigen has distinct surface features that are recognized by the immune system. An antibody is a Y-shaped protein produced by the immune system in response to exposure to antigens.
The tip of each Y-shaped arm contains antigen binding sites (paratopes) that bind to a specific portion of the antigen’s surface (epitope). This binding helps to eliminate antigens from the body. When infected with SARS-CoV-2, the body produces antibodies that bind specifically to the spike proteins and other antigens to help eliminate the virus. This binding can be harnessed to develop antibody and antigen-based diagnostic tests.
Let’s understand the antigen testing method in brief from our experts:
Dr Shivani Sharma, Vice President, Pathology Services, CORE Diagnostics
There is a clear need for a rapid, point of care, an economical test which is also extremely sensitive. Most rapid antigen tests for SARS CoV2 detect the Spike glycoprotein present on the surface of the virus. These tests ensure faster case detection and the quick institution of management and isolation protocols. However, the current antigen tests suffer from low sensitivity.
Also read: ‘Microbiologists playing a significant role in the fight against COVID-19’
While the quest for a sensitive test continues, rapid antigen tests have good specificity, thereby ensuring that patients who test positive in this test are true positives. The ICMR and AIIMS, New Delhi evaluation of one of the antigen tests have found the sensitivity to range between 50.6 percent to 84 percent. This translates to a false negative rate of 16 percent to 49.4 percent which makes testing of negative samples by RT PCR a necessary eventuality to find out if the patient is actually free of the virus.
Operational requirements for the test require stringent temperature control, between two and 30 degrees centigrade. The sample which is a nasopharyngeal swab is collected in an extraction buffer provided by the kit.
The testing methodology is simple and involves the addition of a few drops of the extraction buffer with the patient sample to a lateral flow cassette similar to rapid diagnostic tests for other infectious diseases.
In a nutshell, the rapid antigen test is a useful supplementary test. Surveillance is a key component in our battle against COVID-19 and the rapid antigen test can prove to be very useful. However, it cannot be used independently of the RT PCR test due to its low sensitivity. It can aid on-field diagnosis but might have a limited role to play in the global strategy of “test, trace and isolate.
Point-of-Care testing is need of the hour, says Dr Caesar Sengupta, Vice President, Operations, Thyrocare Technologies
Owing to the increasing numbers of COVID positive cases, entire health system of our country is completely devoted to fast track the testing strategy with the focus on Test, Track and treat immediately. In view of this, ICMR has recently added newer additional testing strategies to ramp up the diagnostic process. This includes Rapid Point-of-Care (PoC) Antigen detection test. This Rapid PoC Antigen detection test must be used in combination with rRT-PCR assay for confirmation. This may be a boon for our country in rapid detection of SARS-CoV-2 virus on-site and to put a stop on further infection spread. However, more data would be required on this to give any statement on its effectiveness. Data available till date shows that such tests (Rapid antigen test) have relatively moderate sensitivity but high specificity.
If a patient is positive by rapid PoC antigen test, that should be considered as true positive and further action should be immediately taken. Whereas, if a patient is symptomatic and has come negative in rapid antigen test, then further confirmation by real-time PCR test is a must.This is very easy to conduct and interpretation can be done by naked eye. Hence, it does not need any special infrastructure or instrument, and can serve as a promising method for rapid diagnosis of SARS-CoV-2, which is actually the need of the hour.
Now, coming to the point that who can be actually benefited by this! It will be highly useful in the hotspots or containment zones or in hospitals, but in combination with the gold standard rRT-PCR test for COVID-19.
People who are living in containment zones and are symptomatic, or asymptomatic but are direct and high-risk contacts of a laboratory confirmed case with underlying comorbidities(tested once between day 5 and day 10 of contact), or anyone seeking hospitalization for essential treatment. It is also beneficial for healthcare individuals, or any other from vulnerable groups who are at high risk.
Having said that, Thyrocare is also prepared to do this assay using ICMR validated and approved kit (Standard Q COVID-19 Ag kit, SD Biosensor).
Sample required for this technique is only nasopharyngeal swabs that should be collected only by trained healthcare worker by following recommended safety measures. Tests should be performed within one hour of collection and real time reporting must be done. We are also partnering with BMC in this initiative of Rapid Antigen Test based screening.
Dr Rashmi Khadapkar, Sr Research Scientist, SRL Diagnostics explains all about the Antigen-based Testing for COVID-19
Testing has become a vital part of the response to the COVID-19 pandemic. As the numbers are continuously on the rise, the government has started looking for ways to scale up the ongoing COVID-19 testing in India by introducing tests like Antigen-based in addition to the gold standard RT-PCR. Since the beginning of the outbreak, RT-PCR is the only recommended diagnostic test for COVID-19. For this molecular test, swab samples need to be collected in a stabilising media, then transported to a laboratory for analysis. RT-PCR though highly sensitive and specific, is technically demanding, requires specialized infrastructure and takes several hours to generate results.
On the other hand, immunoassays for the detection of the antigens or antibodies have been mainstay for screening, diagnosis and management of several infectious diseases. Antigen tests particularly have long been used to detect infectious agents that are difficult, slow, or hazardous to culture.Similar to molecular tests, antigen is a direct test for detection of specific protein or glycoprotein (antigen) for specific microorganism/pathogen. Antigen tests are usually available in rapid test format and can detect viral antigen by the immobilized coated SARS-CoV-2 antibody on the device. The test results of rapid antigen test can be interpreted without specialized instruments and results are available within 30 min. Since antigen tests don’t amplify their protein signal, they are inherently less sensitive as compared to gold standard RT-PCR.
Still this test has been highly acclaimed by experts for speeding up the test-track-treat process. Antigen based tests are easy and cheaper to administer at any site/location. Another advantage is scalability particularly in the current pandemic situation. Results are available within 30 minutes therefore enables quick isolation of positive patients before they risk infecting others It’s important to note that an antigen test reveals if a person is currently infected with SARS-CoV-2 virus. The testing is done through swabbed nasal samples that can help identify if a person has come in contact with SAR-CoV-2 virus. Due to the low sensitivity as compared to RT-PCR, antigen tests are recommended only for high-risk/symptomatic/hospitalized cases from containment zones. Further to avoid false negative results, anyone who tests negative for COVID-19 by rapid antigen testing should certainly be sequentially tested by RT-PCR to rule out infection. In comparison with RT-PCR, specificity of antigen test is good and therefore a positive result need not be confirmed by RT-PCR test and should be considered as a true positive result.
Symptomatic patients with influenza like illness (ILI) and asymptomatic high risk contacts of a positive case with other chronic systemic illnesses, are eligible for the test. In the hospital setting, in addition to patients with ILI, asymptomatic cancer patients, immunosuppressed individuals, elderly patients with other ailments (>65 years) and those undergoing surgeries/ procedures, which generate aerosol shall be eligible for the test. Though not perfect, rapid antigen testing is expected to fill an important gap in current testing protocol by providing quick diagnosis on-site particularly in resource poor settings. Moreover when combined with more accurate RT-PCR, antigen testing can aid in ramping up testing in India.
Be a part of Elets Collaborative Initiatives. Join Us for Upcoming Events and explore business opportunities. Like us on Facebook , connect with us on LinkedIn and follow us on Twitter , Instagram.
Disclaimer: The views and opinions expressed in this article are solely those of the author and do not necessarily reflect the official policy or views of any organisation. The content is intended for informational and educational purposes only and should not be construed as medical advice.
"Exciting news! Elets technomedia is now on WhatsApp Channels Subscribe today by clicking the link and stay updated with the latest insights!" Click here!




















