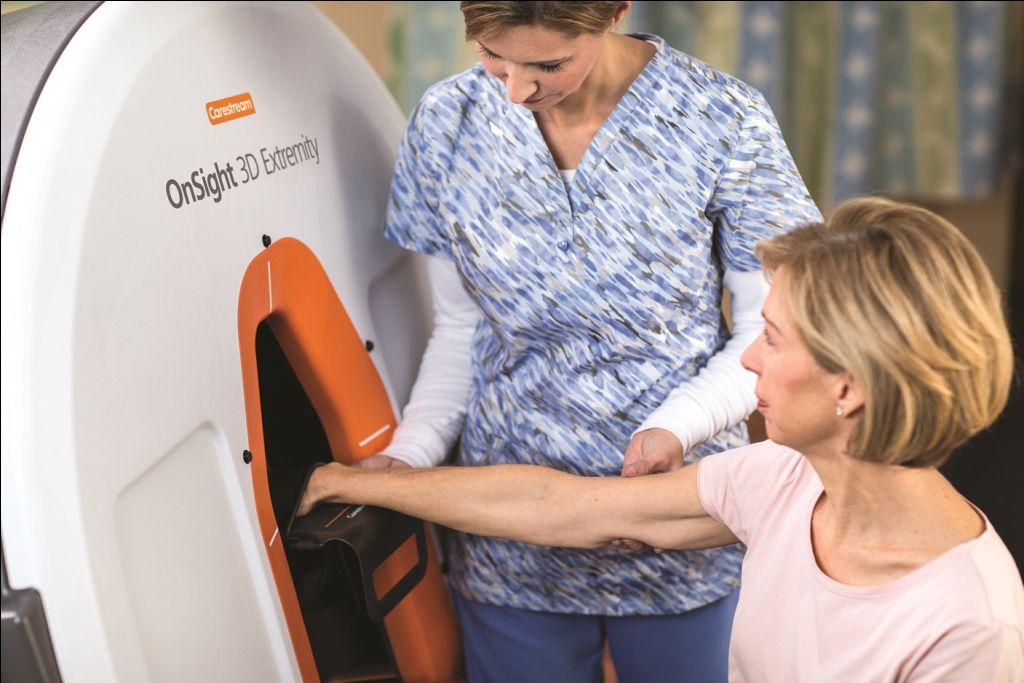
24th March World TB Day
TB is one of the leading causes of mortality in India- killing -2 persons every three minute, nearly 1,000 every day. Every patient who is cured stops spreading TB, and every life saved is a child, mother, or father who will go on to live a longer, TB-free life.
TB is an infectious bacterial disease caused by Mycobacterium tuberculosis, which most commonly affects the lungs. It is transmitted from person to person via droplets from the throat and lungs of people with the active respiratory disease.
Indias Revised National TB Control Programme is the largest TB Control Programme in the world, placing more than 100,000 patients on treatment every month.In healthy people, infection with Mycobacterium tuberculosis often causes no symptoms, since the person’s immune system acts to wall off the bacteria. The symptoms of active TB of the lung are coughing, sometimes with sputum or blood, chest pains, weakness, weight loss, fever and night sweats. Tuberculosis is treatable with a six-month course of antibiotics.
Frequently Asked Questions
1. What is tuberculosis?
Tuberculosis (TB) is an infectious disease caused by a bacterium, Mycobacterium tuberculosis.
2. How is tuberculosis caused?
TB is spread through the air by a person suffering from TB. A single patient can infect 10 or more people in a year.
3. What are the symptoms of tuberculosis?Common symptoms of tuberculosis are: Cough for three weeks or more, sometimes with blood-streaked sputum, Fever, especially at night, Weight loss, Loss of appetite
4. Benefits of DOTS/ Why DOTS?More than doubles the accuracy of TB diagnosis.
Its success rate is up to 95%.
It prevents the spread of tuberculosis by prioritizing sputum positive patients for diagnosis and treatment, thus reducing the incidence and prence of TB.
It helps in alleviating poverty by saving lives, reducing the duration of illness and preventing new infectious cases.
It improves the quality of care and removes stigma.
It prevents treatment failure and the emergence of MDR-TB by ensuring patient adherence to treatment and uninterrupted supply of anti -TB drugs.
It lends credence to TB control efforts and the health system.
5. What is DOTS being implemented?
The DOTS strategy is in practice in more than 180 countries. By March 2006, India has extended DOTS to the entire country.
6. What is the RNTCP?
RNTCP is Revised National Tuberculosis Control Programme (RNTCP) applying the principles of DOTS to the Indian context.
7. How many people die from TB in India every year?
TB is one of the leading causes of mortality in india. It kills more than 300,000 people in India every year.
8. Which is the strongest risk factor for tuberculosis among adults and how does it affects the spread of TB?
The Human Immunodeficiency Virus (HIV, the virus that causes AIDS) is the strongest risk factor for tuberculosis among adults. Tuberculosis is one of the earliest opportunistic diseases to develop amongst persons infected with HIV. HIV debilitates the immune system increasing the vulnerability to TB and increasing the risk of progression from TB infection to TB disease. An HIV positive person is six times (50-60% life time risk) more likely of developing TB disease once infected with TB bacilli, as compared to an HIV negative person, who has a 10% life-time risk.
9. Can tuberculosis be cured in HIV co-infection?
Tuberculosis can be cured, even among HIV-infected persons. TB treatment with DOTS reduces the morbidity and mortality among people living with HIV.
10. For how long must tuberculosis treatment be taken?
Tuberculosis treatment requires at least 6 months of treatment.
11. What is Multi-drug-resistant tuberculosis?
Multi-drug-resistant tuberculosis (MDR TB) is caused by strains of the tuberculosis bacteria resistant to the two most effective anti-tuberculosis drugs available – isoniazid and rifampicin. MDR TB can only be diagnosed in a specialized laboratory.
12. Why are these terms not yet recognised by WHO?
Terms such as totally drug resistant have not been clearly defined for tuberculosis. While the concept of total drug resistance is easily understood in general terms, in practice, in vitro drug susceptibility testing (DST) is technically challenging and limitations on the use of results remain: conventional DST for the drugs that define MDR and XDR-TB has been thoroughly studied and consensus reached on appropriate methods, critical drug concentrations that define resistance, and reliability and reproducibility of testing.[9] Data on the reproducibility and reliability of DST for the remaining SLDs are either much more limited or have not been established, or the methodology for testing does not exist. Most importantly, correlation of DST results with clinical response to treatment has not yet been adequately established. Thus, a strain of TB with in vitro DST results showing resistance could in fact, in the patient, be susceptible to these drugs. The prognostic relevance of in vitro resistance to drugs without an internationally accepted and standardised drug susceptibility test therefore remains unclear and current WHO recommendations advise against the use of these results to guide treatment.
Lastly, new drugs are under development, and their effectiveness against these totally drug resistant strains has not yet been reported.
For these reasons, the term totally drug resistant tuberculosis is not yet recognised by the WHO. For now these cases are defined as extensively drug resistant tuberculosis (XDR-TB), according to WHO definitions.
13. What is the duration of treatment of Multi-drug-resistant tuberculosis?
Multi-drug-resistant Tuberculosis requires at least 18-24 months of treatment with medicines which are 100 times more expensive and often highly toxic.
14. What does the WHO recommend should be done to address MDR or XDR-TB?
The discovery of patients with MDR or XDR-TB emphasizes the importance of ensuring that all care for tuberculosis, whether in the public or private sector, must conform to international standards in order to prevent the emergence of drug resistance. Almost all countries must, in addition, ensure appropriate diagnosis and treatment of cases of MDR-TB. National regulations for the quality and dispensing of anti-TB drugs, particularly of the second-line drugs, need to be strictly enforced.
To achieve this, most countries require simultaneous scale-up of the diagnostic and treatment services for drug-resistant TB, and the provision of adequate and continuous supplies of quality assured SLDs for both MDR- and XDR-TB to meet the increased demand.
MDR and XDR-TB raise many difficult issues concerning the management of patients, for example, whether to isolate patients, the need for institutional, palliative or end-of-life care, and the compassionate use of new drugs. The reader is referred to the WHOs Guidelines for the programmatic management of drug-resistant tuberculosis.
15. Are there any treatment options for patients with XDR-TB?
XDR-TB severely reduces the options for treatment, but, yes, there are still options available, although they have not been studied in large cohorts. For such cases additional drugs will need to be procured from among the group of agents that are known to have some action against tuberculosis but are not routinely recommended for treatment of MDR-TB. These include clofazimine, linezolid, amoxicillin/clavulanate, thioacetazone, imipenem/cilastatin, clarithromycin and high-dose isoniazid. Efficacy is not assured, however, and both toxicity and cost for some of these compounds are high. Potential purchasers should be aware that international availability of some of these agents is limited at present.
16. Will the new drugs in development soon be available for treatment of XDR-TB?
Several new drugs belonging to new classes of anti-mycobacterial agents are under development, but until they are shown to be effective in properly conducted clinical trials, WHO cannot recommend their routine use. In particular WHO advises strongly against simply adding a single new drug to a failing regimen. The use of experimental drugs outside clinical trials (compassionate use) has been addressed by the WHO
PREVENTIVE MEASURES “ Lets join hands to stop TB
TB can affect anyone. If you have cough for more than 2 weeks, get your sputum examined at the nearest designated microscopy centre.
Stay away from TB, not TB patients. They need your love, affection and care to fight TB.
TB is a curable disease. The DOTS treatment provides sure cue for TB patients and is freely available.
People living with HIV (PLHIV) have more chances of developing TB. They should be screened at DMC regularly.
Always cover your mouth with a handkerchief while coughing.
Be a part of Elets Collaborative Initiatives. Join Us for Upcoming Events and explore business opportunities. Like us on Facebook , connect with us on LinkedIn and follow us on Twitter , Instagram.
"Exciting news! Elets technomedia is now on WhatsApp Channels Subscribe today by clicking the link and stay updated with the latest insights!" Click here!