Fighting Pain
 Neurostimulation delivers low voltage electrical stimulation to the spinal cord or targeted peripheral nerve to block the sensation of pain. One theory, the Gate Control Theory of pain developed by researchers Ronald Melzack and Patrick Wall, proposes that neurostimulation activates the body’s pain inhibitory system. According to this theory, there is a gate in the spinal cord that controls the flow of noxious pain signals to the brain. The theory suggests that the body can inhibit these pain signals or “close the gate” by activating certain non-noxious nerve fibers in the dorsal horn of the spinal cord. The neurostimulation system, implanted in the epidural space, stimulates these pain-inhibiting nerve fibers, masking the sensation of pain with a tingling sensation (paresthesia).
Neurostimulation delivers low voltage electrical stimulation to the spinal cord or targeted peripheral nerve to block the sensation of pain. One theory, the Gate Control Theory of pain developed by researchers Ronald Melzack and Patrick Wall, proposes that neurostimulation activates the body’s pain inhibitory system. According to this theory, there is a gate in the spinal cord that controls the flow of noxious pain signals to the brain. The theory suggests that the body can inhibit these pain signals or “close the gate” by activating certain non-noxious nerve fibers in the dorsal horn of the spinal cord. The neurostimulation system, implanted in the epidural space, stimulates these pain-inhibiting nerve fibers, masking the sensation of pain with a tingling sensation (paresthesia).
Source:https://www.medtronic.com/neuro/paintherapies/pain
_treatment_ladder/neurostimulation/neuro_neurostimulation.html
The first recipient of the Eon Mini – the world’s smallest and longest-lasting, rechargeable neurostimulator to treat chronic pain of the trunk or limbs and pain from failed back surgery, was Adam Hammond. Hammond was skydiving in 2006 when his parachute did not deploy correctly. He hit the ground at a speed in excess of 45 miles an hour.
Even with its small size, the Eon Mini neurostimulator has the longest-lasting battery life of any rechargeable spinal cord stimulation (SCS) device in its class. It is the only small rechargeable neurostimulator to receive a 10-year battery life approval by the U.S. Food and Drug Administration (FDA). For patients, this means the device should provide sustainable therapy and maintain a reasonable recharge interval for 10 years of use at high settings. The device’s battery longevity also means that patients require fewer battery replacement surgeries. The charging system is fully portable.
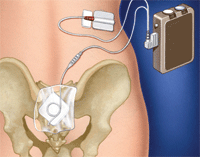
Pain management through neurostimulation systems work in two ways. One is surgically implanted and completely internal and the other has both internal and external components. In an internal neurostimulation system, the battery and lead(s) are surgically implanted something like a pacemaker. In the external kind, a radio-frequency receiver and leads are implanted, and the power source is worn externally with an antenna over the receiver. The advantage of the external system is that it uses an ordinary 9 volt battery which can be replaced.
It should be noted that neurostimulators work to reduce and not to eliminate pain. Certain chronic pain patients have experienced at least 50% reduction in pain upon adopting this line of treatment. It has also been shown to increase activity levels and reduce the patients’ dependence on painkilling drugs. The use of neurostimulators to treat pain must be done very selectively. Proper patient selection and patient education is a must. According to Dr. Ken Follet, University of Iowa Hospitals and Clinics, Neurostimulation is also known as modulation of the nervous system. Rather than ‘cutting’ off specific nerves or blocking signals altogether, neurostimulation actually activates other nerve fibers, which are in fact, pain-inhibiting. Once activated, these pain-inhibiting fibers actually mask the strength of the pain signal reaching the brain, overall leading to less pain being felt.
The device consists of multiple electrodes on a wire that is inserted on the spinal cord and works with a battery. When this is turned on, the device electrically activates nerves in the body and somehow appears to block the transmission of pain signals to the brain. Patients will typically feel a tingling sensation that in a sense masks the pain and after 20 or 30 minutes, they begin to forget about the tingling sensation.
Where it is implanted is based on the location of the pain. The intensity is strictly based upon what the patient feels is comfortable. The patient has his/her own remote control device and can adjust the strength of the stimulation. Another advantage is that it stimulates the secretion of endorphins, improves circulation-especially in the periphery.
Many patients who are being studied for the possibility of applying neurostimulators, have already had multiple surgeries. The most common one being back surgeries for treatment of herniated discs with sciatica. Sometimes patients have had enough. They don’t want to undergo more surgeries. Implanting a neurostimulator does involve a surgical operation, but it is relatively safe and simple. Moreover, as percutaneous placement becomes more prent and multi polar electrodes allow for more targeted stimulation, all applications of neurostimulation are set to become more feasible and less invasive.
Pain is a serious and costly public health issue, and it remains largely under-treated and misunderstood. According to the National Institutes of Health, 90 million people in the U.S. suffer from chronic pain. The American Pain Foundation estimates that chronic pain costs approximately USD 100 billion per year in lost work time and healthcare expenses.
For more of the latest in medical technology visit : www.ehealthonline.org/techtrends
Watch Out ! Don’t lose your balance
 Step into the iShoe – an MIT grad student’s invention could one day prevent falls the aged fear.
Step into the iShoe – an MIT grad student’s invention could one day prevent falls the aged fear.
Your grandmother might have little in common with an astronaut, but both could benefit from a new device an MIT graduate student is designing to test balancing ability.
The iShoe insole could help doctors detect balance problems before a catastrophic fall occurs, says Erez Lieberman, a graduate student in the Harvard-MIT Division of Health Sciences and Technology who developed the technology as an intern at NASA.
Falls among the elderly are common and can be deadly. In 2005, nearly 300,000 Americans suffered hip fractures after a fall, and an average of 24 percent of hip-fracture patients aged 50 and over die in the year following their fracture, according to the National Osteoporosis Foundation.
Lieberman is now testing the iShoe technology in a small group of patients. The current model is equipped to diagnose balance problems, but future versions could help correct such problems, by providing sensory stimulation to the feet when the wearer is off-kilter.
“By doing that we can replace the sense and thus improve people’s balance,” Lieberman says.
Lieberman and other iShoe team members have applied for a patent on the technology, to be jointly held by MIT, Harvard and NASA. In April, the company won a USD 50,000 grant from the Lunar Ventures Competition to help with start-up costs.
Lieberman originally developed the technology to help NASA monitor balance problems in astronauts returning from space.
Zero gravity environments wreak havoc on the vestibular system, one of three body systems that control balance. (The others are vision and sensory receptors called proprioceptors, which tell you where your body parts are in relation to other body parts and the outside world.)
“The change in gravity really screws with their sense of balance. They’re falling all over the place,” says Lieberman, who is a Hertz Fellow and also receives funding from the National Science Foundation and Department of Defense.
The effect usually lasts about 10 days, but NASA tests astronauts’ balance for 16 days after their return. Astronauts go into a phone-booth-like box, where they undergo a series of balance tests such as platform shifts and wall shifts.
While at NASA, Lieberman developed a new system for gathering data and an algorithm to analyse the data.
“We’ve developed the first algorithm that is really capable of not just looking at the pressure distribution of proprioceptors on the feet but also analysing what that’s saying,” he says.
Lieberman soon realised that the technology could reach a wider audience than just astronauts. His own grandmother suffered a bad fall several years ago, and he theorised that a balance diagnostic could help doctors catch balance problems before such a fall occurs.
“You have a gradual progression of loss of balance, osteoporosis, and other factors that can lead to the fall,” Lieberman says.
The iShoe insole would measure and analyse the pressure distribution of the patient’s foot and report back to their doctor. The device could also be outfitted with an alarm that would alert family members when a fall has occurred.
Lieberman and his colleagues are now testing the device in about 60 people, hoping to generate data that will help them create a model to predict the risk of a fall.
Other members of the iShoe team are Katherine Forth, a former NASA postdoctoral associate; Ricardo Piedrahita, a graduate of University of California at San Diego; and Qian Yang, a Harvard undergraduate.
Source: https://web.mit.edu/newsoffice/2008/i-shoe-0716.html
Be a part of Elets Collaborative Initiatives. Join Us for Upcoming Events and explore business opportunities. Like us on Facebook , connect with us on LinkedIn and follow us on Twitter , Instagram.
"Exciting news! Elets technomedia is now on WhatsApp Channels Subscribe today by clicking the link and stay updated with the latest insights!" Click here!










