Web 2.0 and other similar technologies are making the world a smaller more accessible space. This bodes well for the healthcare environment. The content rich domain of medical science needs this open source, increased access and connectedness more so than any other.
 Intel has described eHealth as “a concerted effort undertaken by leaders in healthcare and high-tech industries to fully harness the benefits available through convergence of the internet and healthcare”. A more encompassing definition is provided by Gunther Eysenback, editor of the Journal of Medical Internet Research. He says, “E-health is an emerging field in the intersection of medical informatics, public health and business, referring to health services and information delivered or enhanced through the Internet and related technologies. In a broader sense, the term characterises not only a technical development, but also a state of mind, a way of thinking, an attitude and a commitment to networked, global thinking, to improving healthcare locally, regionally and worldwide by using information and communication technology.”
Intel has described eHealth as “a concerted effort undertaken by leaders in healthcare and high-tech industries to fully harness the benefits available through convergence of the internet and healthcare”. A more encompassing definition is provided by Gunther Eysenback, editor of the Journal of Medical Internet Research. He says, “E-health is an emerging field in the intersection of medical informatics, public health and business, referring to health services and information delivered or enhanced through the Internet and related technologies. In a broader sense, the term characterises not only a technical development, but also a state of mind, a way of thinking, an attitude and a commitment to networked, global thinking, to improving healthcare locally, regionally and worldwide by using information and communication technology.”

eHealth has demonstrated the ability to maximise health care access by extending the reach and quality of healthcare services to consumers as well as by improving the knowledge and skills of healthcare professionals irrespective of place of practice. Perhaps more importantly, it had contributed significantly to the ability of individuals to manage their own health and illness through access to knowledge, training and disease support groups.
Universal Access to Specialised Services
Teleconsultation has provided a means of providing access to specialists (and specialised services) where such access is not easily available. A good example of this is in India where, despite a relatively late start, rapid deployment has occurred due to an enlightened business model, satellite services being provided free by the Indian Space Research Organisation. In many countries which had some initial success, failure to address the high costs of broadband access have resulted in subsequent under-utilisation. An over-dependence on teleconsultation champions has been another problem, proving to be a roadblock to more extensive use of this technology. Some low-end teleconsultation services using email with multimedia attachments to support, store and forward telemedicine services continue to thrive and expand, and in more than a few instances supporting international collaboration in healthcare. Telepathology, teleradiology and teledermatology continue to grow and by their nature are suitable for second opinion referrals. Interestingly in some countries, the initial emphasis on using teleconsultation to support services like telepsychiatry, telenephrology and telepaediatrics has been replaced by the use of these systems to support educational activities and administrative meetings.

From Episodic to Continuous Healthcare Services
Networked health systems and consumer access to the Internet now provide a means of moving from the model of episodic contact between consumers and healthcare providers to a model of continuous relationship more in keeping with the health requirements of consumers. Episodic care was appropriate when most morbidity and mortality arose from infectious diseases, but it is now no longer appropriate when diseases of lifestyle (such as ischaemic heart disease, strokes, diabetes, cancer, injuries and HIV) have become the major causes of illness and death.
Consumers are demanding more access to their healthcare providers, and surveys have demonstrated that modern consumers would like e-mail access to healthcare providers and would be prepared to change their healthcare providers to achieve this link.
The Internet also permits expansion from the business of episodic illness care to well-being management, health risk factor management and chronic disease management, all of which are better served by providing more sustained support for the consumer than periodic office visits. Healthcare consumers are also benefiting from the electronic linkages between healthcare providers and health facilities with their drug and equipment suppliers, as well as with health maintenance organisations and health insurance companies, in ensuring better drug and equipment inventory control and facilitated payments. E-prescriptions have made it possible to ensure continuity of drug supplies for chronic diseases without necessarily having to revisit a distant specialist or health facility.
Linking Businesses and Consumers
Many of the earlier developments in eHealth were driven by the needs of industry, especially those companies involved in the pharmaceutical and medical supply areas, as well as those working in health insurance and other payers. However, other players are now coming on board these business-to-business (B2B) platforms including government agencies and health maintenance organisations.
Some of these agencies have recognised the benefits of developing business-to-consumer (B2C) links through home pages based on the Internet, e-mail and call centres in terms of improving services and developing customer loyalty. Consumers have also discovered for themselves that the Internet is a great medium for developing consumer-to-consumer (C2C) links through disease support pages and health discussion groups on the Internet maintained by support groups or individuals.
The manner in which Internet discussion groups have empowered individuals with rare diseases and parents of children with uncommon conditions is a striking example of the benefits of eHealth for consumers. More information is available from these sites than could possibly be conveyed during the short office visits with their doctors. Answers to specific queries are quickly available from other consumers, and while such information is not uniformly credible, discriminating consumers can find much to help them.
By visiting these pages, the health industry and healthcare providers who are not leveraging the benefits of eHealth could learn about the power of electronic networking to extend their reach and the repertoire of services provided.
Electronic Lifetime Health Records and Lifetime Health Plans (or Personalised Health Records)
Many of these eHealth initiatives have been ad hoc and driven by industry or concerned consumers, but many countries recognised the need for coordinated eHealth initiatives. In 1997, Malaysia published its Telehealth Blueprint: Transforming Healthcare through Information Technology, the aim of which was to transform the healthcare system and realise the vision of a ‘nation of healthy individuals, families and communities’ using information technology as a powerful enabler to build a system that is fundamentally consumer-centric.
An electronic lifetime health record for every citizen forms the core of this deliverable service. Such records will provide a means for the consumer to share their health records with those health providers they visit over the course of a lifetime in public and private health facilities. Health and illness will be managed in a proactive and forward-looking manner, with periodic health visits rather than episodic ‘one-off’ visits when illness strikes.
Each visit will result in updating the personalised health plan and ensuring ‘seamless, coordinated, continuing’ care. This can be especially valuable in the management of health risk factors and chronic diseases. In these circumstances, shared medical summaries could ensure seamless continuity of care, avoid unnecessary duplication of investigations and reduce dangerous drug interactions. Technologies that can further enhance the value of eHealth centred-on electronic health records and plans are identified in Figure 1 below.
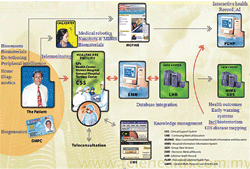
Figure 1: Enhanced eHealth Services
Australia and the UK have subsequently published their national blueprints, both of which also centre on coordinating healthcare services through the use of nationally shared lifetime health records. Both countries have also launched national consumer health portals, with the UK’s portal being supported by a national telephone call centre manned by trained nurses. Similar consumer health portals launched by governments exist in Malaysia, Singapore and other countries. In Asia, eHealth strategies of varying degrees have also been developed at national level in Hong Kong, Singapore, Japan and South Korea.
All players in the healthcare system should be linked to achieve optimal results including:
-
Consumers – via patient identifiers, smart cards, home monitoring systems and access to their own personal health records, into which they may enter observations.
-
Healthcare providers and facilities – through national health information networks, which may include total hospital information systems and total health information systems, teleconsultation hubs and continuing professional development portals.
-
The Government – through the information derived from aggregated patient data in electronic health records (which can be used to support health planning and financing) and early warning systems for acute illnesses and prence reports for chronic disease.
-
Health insurance and other payers – through e-commerce and group data services.
-
Pharmaceutical and medical equipment companies – through electronic inventory control and just-in-time supplies.
-
Professional medical societies – through Internet-empowered continuing professional education support and credentialing activities.
-
Medical faculties – in providing distance education for the different categories of health professionals and support for acquiring post-basic, undergraduate or postgraduate qualifications.
-
Social welfare bodies – in providing support for disadvantaged patients.
-
Disease support groups – in extending their reach to their respective constituencies.
Geography and time need not be barriers to achieving high-quality care. A distant specialist, a rarely used drug, authorisation for payment or a clinical practice guideline need only be a click away. With the development of wireless networks and handheld computers, such services can reach the consumer or healthcare provider at all times. A summary of the health record has been incorporated into the national smart card in Malaysia, allowing consumers to carry relevant health information with them wherever they go. Life vests that monitor vital signs and sends them to a central health facility have been developed, as also a wrist watch that monitors vital signs. These, linked to geographical information systems, have been made available to army personnel working in difficult areas like Afghanistan and Iraq.
Ensuring Patient Safety and Better Health Outcomes
The US Institute of Medicine has re-emphasised the morbidity and mortality that results from pharmaceutical drug use. In the USA alone, more than a million injuries and as many as 98,000 deaths each year can be attributed to medical errors. Decision support can be built into these lifetime health record systems to permit just-in-time information to ensure good clinical care.
With almost 10,000 different diseases and syndromes, 3000 medications and 1100 laboratory tests to select from, the average doctor requires some help in managing his patients. Keeping up to date is a herculean task, with 400,000 articles added to the medical literature every year. A continuing medical education portal for healthcare providers and a consumer health portal are needed to ensure consumer and provider access to accredited health information. This should be linked to electronic health record systems to ensure just-in-time decision support and enhance patient safety.
From eHealth to Medicine 2.0
A very exciting and significant development for eHealth has been the adoption of web 2.0 technologies and approaches in what has been called Medicine 2.0 or Next Generation Medicine. Medicine 2.0 has been defined as Web-based services for healthcare consumers, caregivers, patients, health professionals and biomedical researchers that use Web 2.0 technologies and/or semantic web and virtual reality approaches to enable and facilitate social networking, participation, apomediation, openness and collaboration, within and between these user groups. This has coincided with the recent emergence of Personal Health Application Platforms and Personally Controlled Health Records such as Google Health, Microsoft HealthVault and Dossia.
Social networking (modelled on Facebook and similar applications) will allow health consumers to see and share what those with similar diseases are doing and reading on the Internet, foster viral dissemination of information and skills, and enable reputation and trust management and accountability and quality control. Social networking tools for health may get people interested in personal health records which they need to actively maintain (like their profile in Facebook), motivate them to take responsibility for their health and health information and, especially important, retain their interest over time. The philosophy of end-user participation and engagement is deeply engrained in Web 2.0 thinking, exemplified by tools like wikis. Patient access to and control over their own health data is probably an important pre-requisite to engaging him in the management of lifestyle risk management and chronic disease care. The emergence of social networking platforms and applications such as PatientsLikeMe, combined with Personal Health Records 2.0 create unique levels of participation and opportunities for engaging patients in their health, healthcare, and health research, and for connecting patients with their caregivers, formal and informal. Apomediation (use of informed or experienced agents to guide patients to high quality information or services), as opposed to disintermediation (cutting out the middleman), is supported by the Web 2.0 environment. Openness (as exemplified by transparency, interoperability, open source and open interfaces) and collaboration are important in eHealth development and are well supported by Web 2.0 applications.
In conclusion, not only is eHealth well and thriving but the best is yet to come in addressing the goals of better healthcare access and health outcomes. 
Be a part of Elets Collaborative Initiatives. Join Us for Upcoming Events and explore business opportunities. Like us on Facebook , connect with us on LinkedIn and follow us on Twitter , Instagram.


