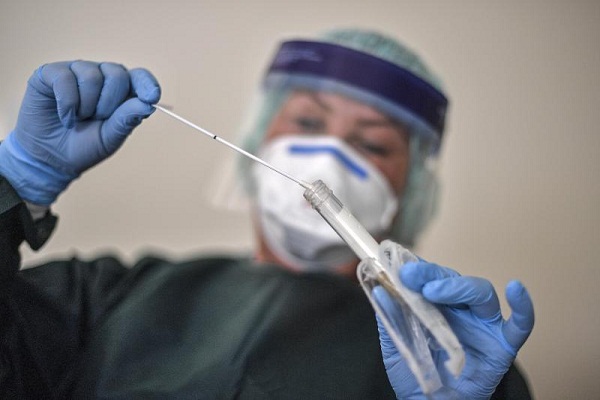
Dr Kashmira Limaye, Consultant Clinical Microbiologist and Infection Prevention Specialist of Jupiter Hospital, details about the challenges and day to day comprises of the microbiologists are going through battling out the infectious microorganisms.
My work involves testing clinical samples for infectious microorganisms like various bacteria,viruses, parasites and fungi. It also involves formulating Hospital infection control protocols and monitoring their compliance. Owing to the nature of our work, lab personnel like me come in direct contact with infectious microorganisms. Despite following standard precautions while handling and processing infectious samples, we are at a continuous high risk of contracting infection.
COVID 19 pandemic, caused by a novel coronavirus (SARS CoV2), has spread across the globe infecting more than 12 million people worldwide. In India the numbers have crossed seven lakhs and are still counting. Considering Indian population, the pressure on healthcare is huge and dealing with SARS CoV 2 has been a completely different experience. Its contagious nature and associated fatality have led to panic even amongst healthcare professionals. With more than hundred doctors succumbing to it and many more infected, appropriate precautions are a necessity.
Also read: Biocon drug for COVID 19 ALZUMAb® (Itolizumab) to cost Rs 7,950 per vial
As part of the hospital infection control team, proper planning and strict implementation of infection control measures throughout the hospital is my responsibility which involved training, segregation, monitoring, diagnosis etc.
Precaution ‘need of the hour’
Our team started with training all healthcare staff including doctors, nurses, housekeeping staff, maintenance staff about general information about the virus, modes of transmission, hand sanitization, disinfection of surfaces, biomedical waste segregation, precautions to be taken at work and at home and importance of Personal Protective Equipment (PPE).
Protocols were set in line with International and Indian Council of Medical Research (ICMR) guidelines and strict compliance was ensured .
Go into detail
Fever OPD with dedicated entrance and exit of suspected patients was set up to avoid mixing of patients. Protocols were laid down to segregate inpatients limiting chances of cross infection.
Diagnosis and its challenges
Prompt and accurate diagnosis with early isolation of infected patients is the key to manage and limit transmission effectively. Unfortunately, not all patients present with typical symptoms making clinical diagnosis difficult. The Reverse transcription-polymerase chain reaction (RT-PCR) test, which is the gold standard for definitive diagnosis, is technically a complex test. It requires expertise in molecular biology and a well-equipped laboratory with appropriate infrastructure to minimize cross contamination like negative pressure room, Biosafety cabinets etc.
Setting up the PCR lab was a challenge as it needed to be rapid and efficient without compromising on quality. Following the approvals from National Accreditation Board of Laboratory Testing (NABL) and ICMR we started COVID 19 testing.
Sample collection and transport
Nasal and throat swabs are the samples that are collected and transported in a Viral Transport Medium (VTM) to ensure its viability. SARS-CoV 2 is an RNA virus which makes it unstable. Appropriate sampling, strict cold chain maintenance and triple packing to avoid spill of contaminated medium are crucial preprocessing steps.
Doctors and technicians collecting swabs have to wear PPE that includes a gown, surgical mask, surgical gloves, an N95 mask, shoe covers and goggles and need to follow hand hygiene strictly at all times.
In the microbiology lab, the actual processing is done in biosafety cabinets to prevent contamination and infection. Before entering the PCR lab our technicians wear full gear of PPE. RT-PCR test involves viral RNA extraction and amplification. Extraction involves a lot of sample manipulation making it a risk prone step hence requiring extreme precautions. Every step is closely monitored to avoid errors that may lead to exposure or erroneous results.
Donning and Doffing PPE
After donning PPE suit, the personnel have to work in the suit without food, water, or attending to nature’s call which is suffocating and stressful but vigilance is mandatory at all times.
At the end of shift doffing of PPE is done under supervision to avoid protocol breach. It is done systematically and slowly without generating aerosols around and sanitizing oneself several times during the whole process. All our team members are trained in hand hygiene techniques and donning and doffing of PPEs.
The entire process is a tireless team effort and we are committed to round the clock working to deliver results rapidly and accurately. We are holding regular morale boosting sessions to keep the motivation going. Healthy diet, exercise, breathing exercise and rest is stressed upon for good immunity.To avoid passing infections to our loved ones, we maintain distance from our families to keep them safe.
As a ‘silent’ COVID warrior, it’s a matter of pride that my team and I are doing our bit for our country.
Be a part of Elets Collaborative Initiatives. Join Us for Upcoming Events and explore business opportunities. Like us on Facebook , connect with us on LinkedIn and follow us on Twitter , Instagram.
Disclaimer: The views and opinions expressed in this article are solely those of the author and do not necessarily reflect the official policy or views of any organisation. The content is intended for informational and educational purposes only and should not be construed as medical advice.
"Exciting news! Elets technomedia is now on WhatsApp Channels Subscribe today by clicking the link and stay updated with the latest insights!" Click here!




















