Understanding BMI


Body Mass Index
Body Mass Index or BMI is one of the most commonly used statistical tools to measure body fat. Calculated by taking the ratio of individuals weight and height, BMI has seen tremendous prence, over the years, in usage from both individuals and medical community. Its wide reach can be attributed to the fact that it is extremely simple to calculate, reasonably informative, cheap and non-invasive in nature. It is now commonly accepted as a useful screening tool for weight profiling of individuals, as well population groups.

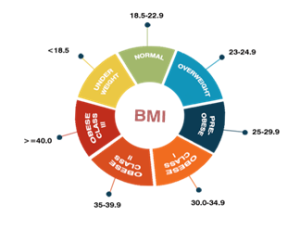
The chart above captures BMI score ranges and corresponding categories
Based on the BMI score, an individual is classified as either underweight, normal, overweight and obese. A score above 25 makes the individual overweight and one above 30 makes her obese.

As BMI has seen prolific use over the years, at AllizHealth, we have done extensive analysis on the issue of understanding the benefits and limitations of BMI. Additionally, we have also delved into the matter of what could be other simple additional measures that can be undertaken by individuals and practitioners to procure improved insights and build sustainable models around weight and body fat management.

Based on a dataset analysis, PAN India, we observed that ~64% people have higher than normal BMI and among them 7% in Obesity level I/II and 1% are severely obese. Based on this classification, overweight and obese individuals are identified as ones carrying high risks of diseases that are typically associated with excess weight and body fat. These would include risks for heart diseases, diabetes (type 2), stroke and hypertension, some types of cancer and kidney disease. Hence, BMI works as an efficient tool to red flag risks associated with excess body fat and weight. The below charts enunciate various insights on populations BMI status, generated from AllizHealths dataset.
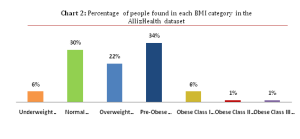
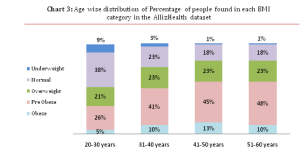
Age wise distribution of Percentage of people found in each BMI category in the AllizHealth data set (Source: AllizHealth Analysis)
BMIs Limitations in Indian Context
While the benefits of BMI are many, it is imperative to look into its limitations, especially in the context of people belonging to Indian/ South Asian ethnicity. It has been increasingly observed that, among Asians, there is strong correlation between lower BMI and higher body fat. Therefore, there is a high probability that even if an individual has lower BMI, s/he might be having high body fat and therefore at risk of several diseases including diabetes and cardiovascular ailments.
This limitation in BMI materialises because it does not take a deeper look into individuals body fat in the context of ethnicity. It tends to skim over the fact that South Asians and Indians have at every BMI level demonstrated higher concentration of fat in the abdominal region, higher degree of insulin resistance, hypertension, and diabetes, culminating into much higher risks for cardiovascular diseases.
For any given BMI, Indians have higher Abdominal Obesity which is an important parameter to determine several metabolic syndrome diseases. A large proportion of urban Indian adults have the metabolic syndrome which increases the risk of both diabetes and cardiovascular diseases. Indians develop diabetes at a lower BMI and waist circumference compared to western countries. From our data set, we observed that only 34% people have their waist size within the normal range, 50% borderline and 16% people have high- very high abdominal obesity (see below).
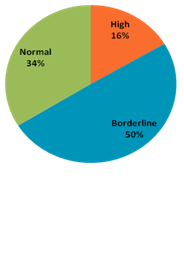
Waist size categories and corresponding percentage of people (Source: AllizHealth Analysis)
Further, gender-based analysis on the issue of waist size shows that 34% of the total female subjects have high abdominal obesity in comparison to 12% male subjects. Out of the total female population only 18% have normal waist size comparison to 38% male. Upon further uation it seems that Indian women after the age of 30-35yrs tend to develop fat around the waist which continues till the latter stage of life (see below).
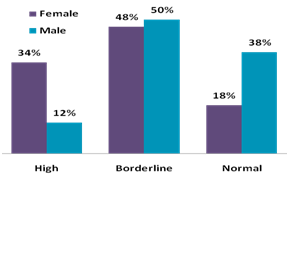
Waist size categories and respective percentage of males & females
We also did analysis on the risk that abdominal obesity poses to various age groups. Majority of the moderate risk and high risk from abdominal obesity was found in the age groups of 21-30 years and 31-40 years (see the below chart). Based on our analysis of PAN India data set analysis, it seems age also plays a vital role in developing abdominal obesity among Indians. May be because after a certain age people in India are less physically active, in terms of doing exercise.
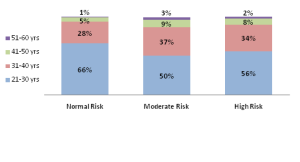
Abdominal obesity risk classification for each age group (Source: AllizHealth Analysis)
What makes Abdominal Fat especially bad?
To understand the dangers of abdominal fat it would be useful to acknowledge that not all body fat is same. The fat that we find below our skin and can be touched is called subcutaneous fat. On the other hand, the fat found in our abdomen is called visceral fat. It is called so because this fat lies in the space around viscera i.e. stomach and intestines. Visceral fat produces and releases a number of toxins into the body. Among these toxins is Cytokines. Cytokines has a number of potential bad effects, namely:
- Increase probability of a cardiovascular diseases and Stroke
- Reduce sensitivity to insulin, bringing on diabetes
- Causing inflammation that can cause cancer of the colon,esophagus and pancreas
- Increase cholesterol levels
For a given weight, it is therefore, much safer to have the fat distributed all over ones body or even concentrated around the hip area versus concentrated in the stomach area.
Identifying Abdominal Obesity
Identifying abdominal obesity is simple and does not require any detailed diagnosis or blood tests. In conjunction with BMI, the following two measurements should be considered:
Waist Circumference (WC): You can measure your waist circumference by placing a tape measure around your body at the top of your hipbone and above your belly button. A measure of more than 35 inches for women and more than 40 inches for men-is considered above normal and indicate abdominal obesity.
Waist Hip Ratio (WHR): It is the ratio of the circumference of the waist and hip. According to WHO, hip circumference should be measured around the widest portion of the buttocks, with the tape parallel to the floor. The WHO states that abdominal obesity is defined as a waist“hip ratio above 0.90 for males and above 0.85 for females.
Conclusion
Given the various data points presented here in the paper, as well as our understanding of various medical research work in the domain, it is now sufficiently clear that in the context of South Asians including Indians the danger of abdominal obesity and its many potential threats is very real. Additionally, BMIs limitation as sole tool to highlight abdominal obesity must be recognized. Necessary additions to existing diagnostic tools (read BMI) must be made by adding the application of WC and WHR. Finally, it is imperative that a holistic approach, consisting of appropriate dietary & lifestyle changes be adapted to reducing and managing abdominal obesity both at an individual and population level.
About AllizHealth
AllizHealth, a healthtech start-up in preventive care space, is a Mumbai Angels funded company and based out of Pune. As part of its initiative, AllizHealth is building a health platform to help people identify their health problems early and then use various resources to track and manage the same. At present, AllizHealth is working with some of the leading insurance and hospital groups in India and managing the health of over 500,000 users. Based on their data (~300,000) users, AllizHealth has done an extensive study on the role played by BMI and the relatively less importance given to the crucial factor of WHR.
About the Authors
Dr Rasmi Mishra (Co-Founder & Chief Data Scientist) has over 24 years of experience in IT and a PhD in Artificial Intelligence. At AllizHealth, she is involved with data analysis and building various predictive health models.
Aditya Roy (Chief Strategy Officer) has over 10 years of experience in the startup space and has helped startups with their fund raise and go to market strategies. At AllizHealth, he handles its partner programs and new market opportunities.
Be a part of Elets Collaborative Initiatives. Join Us for Upcoming Events and explore business opportunities. Like us on Facebook , connect with us on LinkedIn and follow us on Twitter , Instagram.
"Exciting news! Elets technomedia is now on WhatsApp Channels Subscribe today by clicking the link and stay updated with the latest insights!" Click here!