
 Human blood, the life stream of human beings has no alternatives. The need for reliable and safe and uncontaminated blood is still inaccessible for many. The country dwells on a pathetic state where transmission of infectious diseases through blood transfusion is prent. It is a call for an immediate remedy to invigorate the blood banks sector, writes Prathiba Raju of Elets News Network (ENN).
Human blood, the life stream of human beings has no alternatives. The need for reliable and safe and uncontaminated blood is still inaccessible for many. The country dwells on a pathetic state where transmission of infectious diseases through blood transfusion is prent. It is a call for an immediate remedy to invigorate the blood banks sector, writes Prathiba Raju of Elets News Network (ENN).
India requires 12 million units (one unit is about half a litre) of blood every year and the supply is at nine million, there is a dearth of three million unitsa gap of 25 per cent. Adding to this shortage of blood, the fragmented blood banks industry, lack of trained personnel and outmoded screening tests disorders like sickle cell anaemia, thalassemia and haemophilia that require repeated blood transfusions makes the deficit more appalling.

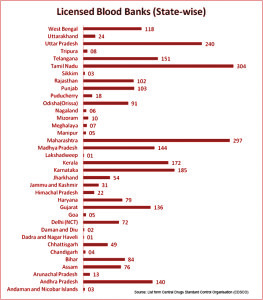
As per the National Health Profile data released by the health ministry recently, India has a total of 2,760 licensed blood banks, with the state of Tamil Nadu, at 304, possessing the highest number, followed by Maharashtra with 297 blood banks and Uttar Pradesh (240). India’s north-eastern states have the lowest number of blood banks with Assam, Nagaland, Mizoram and Manipur having 76, 6, 10 and five blood banks respectively, the data shows. Among the total number of licensed blood banks in India, 1,564 are run privately and 981 by the government.
Blood banks are extremely fragmented in India with too many centres; most are hospital-based. Though the blood policy was adopted by the parliament there has been very little work done after that to implement what is enshrined in the policy. What we need is radical changes moving to centralised blood collection and processing and provision of these units at all hospitals without any pre-condition of replacements, said Dr Aseem Kumar Tiwari, Associate Director and Incharge, Department of Transfusion Medicine, Medanta -The Medicity Hospital, Gurgoan.
As per expert medical practitioners, maintaining a safe blood supply is a challenge in many countries particularly for a country like ours. Reliable blood means safe blood donors, safe blood transfusion practices and rational use of blood.

Safe Blood-A Dire Challenge
 Right from blood transfusions for thalassaemics and haemophiliacs, surgeries after accidents has been a nightmare for few patients, for 10-year-old Aditya, whose parent face a tough time to arrange two unit of A negative blood as he suffers from thalassemia and requires regular blood transfusion.
Right from blood transfusions for thalassaemics and haemophiliacs, surgeries after accidents has been a nightmare for few patients, for 10-year-old Aditya, whose parent face a tough time to arrange two unit of A negative blood as he suffers from thalassemia and requires regular blood transfusion.
My child and many like him are not safe. Despite stricter testing norms, they are still at risk. For each and every transfusion hunting a safe blood is still a dream, says Arpita Gupta, mother of Aditya, and also a member in Thalassemics India, a patient group.
Thalessemic patient between the age of one to five years needs one unit of blood every month, between the age of five to ten-two units every month are needed, between the age of 10 to 15-three units are needed every month. An adult thalassemic needs four units of blood every month.
Annually, unsafe transfusion causes an estimated 8-16 million Hepatitis B infections, 2.3-4.7 million Hepatitis C infections and around 1.6 lakh HIV infections.
Safe blood transfusion is one of the key life-saving interventions that should be available for patients in need. Yet, equitable access to safe blood still remains a major challenge in many countries. Providing safe and adequate supplies of blood and blood products should be an essential part of every country national health care policy and infrastructure, informed Dr Edward Kelley, Director of Service Delivery and Safety at WHO.
National Aids Control Organisation (NACO) informs that access to safe blood is mandated by law, and that is there primary responsibility. The specific objective of the blood safety programme is to ensure reduction in the transfusion associated with HIV transmission to 0.5 per cent, while making available safe and quality blood within one hour of requirement in a health facility. However, there is a serious mismatch between demand and availability of blood in the country: against 12 million units/ year requirement, the availability is only nine million units/year. Another concern is that voluntary blood donation is 52 percent. NACO is committed to bridge the gap in the availability and improve quality of blood under National Aids Control Programme III (NACP III).
Safety during blood transfusion should be considered priority but many blood banks which are operated in grass root levels are not aware of it. Many women get infected during the pregnancy while the blood is transfused. It is mandatory to check blood for HIV before it is banked. There is no possibility of infection if blood is checked and banked properly, Kouslaya Periaswamy, founder Positive Womens Network (PWN) told Elets News Network (ENN).
Assuring the safety of the blood transfused from one vein to another is a rigorous process and it shouldstart from screening of the donors which includes testing, careful quality control of donated blood.
Voluntary Donation In Paltry State Blood is an intrinsic requirement for healthcare and proper functioning of the health system, however everyday hundreds of patient struggle to get blood on time. The procurement of blood on time still depends on the patient relatives and not with the service provider.
“We do not have a proper VBD programme that can run throughout the year to take care of the demands. There have been efforts to improve the VBD but vested interests have marred the progress. The madness to commercialise blood banking is ruining the very concept of VBD, said N K Bhatia, Mission Jan Jagriti Blood Banks, Delhi.
Ironically India is among 51 countries to sign the Rome Declaration on Achieving Self-Sufficiency in safe blood and blood products based voluntary non-remunerated donation. But voluntary blood donation (VBD) is still very low and the majority of the blood donors are family donors or replacement blood donors. Experts stress that only awareness and more sensitisation and enhanced blood donation camps can match the shortage.
The best way to guarantee a safe and adequate supply of blood and blood products for transfusion is to have a good supply of regular donations by voluntary unpaid blood donors, says Dr Margaret Chan, WHO Director-General.
Indian Red Cross Society (IRCS), which contributes 10 per cent blood of the total requirement in the country, says that they start a motivational programme for youth and make them lifelong blood donors.
“IRCS is already in the activity for over 50 years, we motivate the youth an the safest donors as they are free from disease or medical issue like blood pressure. IRCS play auxillary role for the government to get more donors, said Vanshree Singh, Director, Indian Red Cross Society.
According to an NGO, who run blood bank a universal donor card for volunteers would help the VBD. For example, if a donor donates blood in Delhi but he or his family is in need of blood at Bengaluru, there should be a system in place where the donor card he carries be given equal recognition in the other parts of the country. Under the current system, blood donors are issued donor cards by blood banks where they donate the blood at, and they can only approach that bank in case of an emergency. As per estimates, four in a population of 1000 persons in India are blood donors.
Although VBD is still very low and the majority of the blood donors are family VBD and replacement blood donors, the technology like bar coding, scanners and deep freezers are trying to enhance the quality of the donated blood.
Enhancement through Technology
Blood banking needs a balance between safety and efficiency. Technology like bar coding, scanners makes routine tasks easier to perform. The sector has only recently accepted the use of ICT.
Technology helps in traceability and it can checks status of stocks, alerts expired stocks, quarantine management, inventory being sent to storage centres will help in better and effective stock utilisation and supply chain management. With all records available for audit and analysis, better planning and resource allocation can be made. Technology also helps in predictable outcomes and is monitored efficiently. The blood chain stakeholders consist of different players operating in silos bringing them into one umbrella, informed Dr. Rasika Dhawan Setia, Senior Consultant Department of Transfusion Medicine & Hematology, New Delhi.
Bar coding system provides a unique number of the donor blood so it can be easily traced. Nowadays patient wristbands have a bar code which helps to store the data of that individual, chances of mix-up clerical errors are reduced. In blood bags we have the sampling pouches in which the first 15 ml of blood gets collected and sampling is done from which reduces the mix up and bacteria contamination. Deep freezers have chart recorder it is connected to data loggers information connected to central computer, which can be accessed through mobile phones, she added.
Odisha government has started e-blood banks, an integrated blood bank automation system. These banks help with the real-time updates on what type of blood is available in the state blood banks.
India is among 51 countries to sign the Rome Declaration on Achieving Self Sufficiency in Safe Blood and blood products based voluntary nonremunerated donation
This web-based mechanism interconnects all blood banks of the state into a single network and includes elements of acquisition, validation, storage and circulation of various live data and information electronically regarding blood donation and transfusion service. The system developed by Odisha government is a success, said Pramod Kumar Meherda, Mission Director, National Rural Health Mission, Government of Odisha.
While the state government are trying to imbibe new technologies a five-member team has developed a mobile app and a website to match people who need blood with those willing to give it, instantly.
Bloodline Android app can be downloaded from the Google Play Store or register with Bloodlinelabs.com to join the network. Once a request is placed, Bloodline runs algorithms to match potential donors based on location and blood group and notifies only them. The app is a hit in Chennai and Bangalore, said Arun, member Bloodline.
The mobile app helps to contact patients to spot willing donor with apt blood group. Instead of outdated list of regular donors who may or may not be available, he added.
Government will explore the possibility of establishing a mechanism where people can check online the availability of required blood groups in blood banks across the country. The government has taken steps for expanding the infrastructure in blood banks across the country for the benefit of common people, Health Minister J P Nadda inform parliament.
Centralised Blood Banks Needed
Blood banking and transfusion medicine sector needs to transform, all stakeholders must join hands to advocate uniform pricing and highest safety standards for blood and components along with safe transfusion practices, inform experts.
The emphasis should be on adopting IT in blood banking. Blood banking system in India is decentralised, while in Western countries it is centralised. Therefore, we see that blood banks have varied practices of blood manufacturing and using different technology. As the technology advances, the cost of blood components go high, Tiwari added.
For a safe, source and ethical supply of blood, blood products, appropriate and rational clinical use of blood are important as its a responsibility of every government, informed RN Makroo, Director, Department of Transfusion Medicine, Apollo Hospitals, New Delhi.
Be a part of Elets Collaborative Initiatives. Join Us for Upcoming Events and explore business opportunities. Like us on Facebook , connect with us on LinkedIn and follow us on Twitter , Instagram.












