
Our top priority is newborn care and family comfort, therefore our NICU offers high-end quality, expertise and intensive care around-the-clock to each patient, says Dr Amit Jagtap, Neonatologist, Hinduja Healthcare Surgical
What are the key unique facilities and services offered under NICU at your hospital?
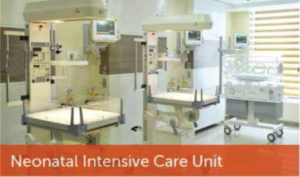
At Hinduja Healthcare Surgical, we have a Neonatal Intensive Care Unit marked with following unique facilities and services. These include a 4 bedded, state of the art, level 3 NICU strategically stationed right besides the labor and delivery room which also has cautiously been built on the same floor as the mothers obstetric-post-natal ward. We provide a fully-equipped neonatal transport incubator which would aid the transfer of neonates, within the hospital premises e.g. from the O.T. to the NICU and vice-versa also between different hospitals. This transport incubator is capable of providing a controlled thermo-neutral environment to the baby it harbors; and prevent any adverse effect of the transport on the babys health. Once stabilized and received from the origin, the incubator provides a hassle-free transfer of the neonate to the destination. Once in our unit, the neonate is collectively looked after by NICU team which comprises of full-time dedicated and experienced neonatologist, pediatricians, neonatal fellows, NICU trained nursing staff, pediatric anesthetists and a lactation consultant.

How do you ensure multidisciplinary connect and expertise at the NICU alongside Pediatrics?
Apart from the above mentioned NICU team, we have an easy access to allied faculties such as a cardiologist equipped with an in-house, bedside 2D echo facility, a pediatric surgeon, promptly available at any emergent occasions. Pediatric and Neonatal anesthetist, for specialized neonatal interventions are also available. In addition, an in-house 24×7 radiology support along with an efficacious and prompt laboratory support with respect to urgent hematological and biochemical uations or decisionmaking cytological and histo-pathological diagnoses is present. The NICU team alerts the concerned allied faculties as per any information that becomes available regarding high risk neonates diagnosed at birth or anticipated based on ante-natal detection.
 What are the latest technologies installed at your NICU?
What are the latest technologies installed at your NICU?
Our NICU proudly displays the suc- Specialty care for Newborns cessful use of the following cuttingedge technologies essential for the care of high risk and sick newborns. These include high frequency oscillatory ventilation (HFOV), use of Laminar flow for the sterile preparation of all medications and IV Infusions. We use neo-puff with air-oxygen blender to minimize iatrogenic lung trauma during resuscitation of the neonate and also have a trans-illuminator device that aids in neonatal intravenous access, in order to minimize the handling of the neonate and the degree of invasion of the babys skin integrity. What is the non-invasive management technologies adopted for newborns? Keeping in mind the need to be as less invasive as possible, in the management of neonates, we A.M.T. our NICU facility always strive hard to look for non-invasive therapies and interventions to be used in the NICU management of neonates. Some of these include trans-cutaneous bilirubin meter for non-invasive estimation of jaundice level in the baby. This is important as
Dr Amit Jagtap
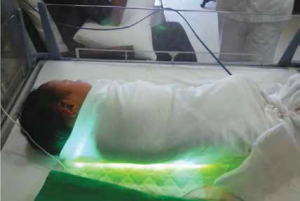
occurrence of jaundice is very common amongst new borns. Secondly, we have non-invasive ventilation in the form of both Continuous positive airway pressure (CPAP) as well as Nasal intermittent positive pressure ventilation (NIPPV). The hospital utilizes capnography for determining carbon-dioxide level in ventilated babies without the need of blood gas analysis. Advanced phototherapy options such as; LED panels and the Bili-blanket which has a Dr Amit Jagtap definite advantage over the conventional modalities with respect to the neonatal outcomes are present A.M.T. our facility. Bili-blanket for hyperbilirubinemia ensures closed contact of the baby to the source of light without the risk of hypothermia as well as the ease of handling and nursing of the baby by the mother without interruption of the phototherapy.

 What are the key steps taken by for infection control at NICU?
What are the key steps taken by for infection control at NICU?
Infection control is critical to the NICU facility and extensive caution and care guidelines are outlined for the same at the hospital. Key steps taken by our NICU for strict Infection control includes strict adherence of the doctors, nursing staff, housekeeping staff as well as the parents to the universal safety precautions with continuous and ongoing earnest reminders regarding the same amongst the members of the NICU team. A 1:1 nurse: patient ratio ensures adequate attention is given to each patient to ensure complete guidance care and monitoring. Other than that for the NICU team, entry into the NICU, allowed only for parents, that too after a thorough understanding imparted regarding implementation of the NICU infection control strategies with vigilant supervision. Strict hand washing techniques has been laid down, also strict policies with respect to wearing of cap-masks and the liberal and appropriate use of hand-sanitizers prior to any handling of the baby are instructed to all. To ensure regular updates and feedbacks are included this is an ongoing activity with regular revision, discussion and improvisation of the policies amongst members in order to find out any breaches in the prevailing system with prompt rectification of the same.
“We provide a fully-equipped neonatal transport incubator which would aid the transfer of neonates, within the hospital premises to the NICU and vice-versa “
 What are the trends in disease case at the NICU in percentage of cases?
What are the trends in disease case at the NICU in percentage of cases?
Trends in disease case at the NICU in percentage of cases have been that the total preterm births are around 40 percent out of which almost 50 percent were in the region of 33 weeks to 36 weeks of term. Prematurity with low birth weight and apnoea of prematurity accounted for almost 21 percent cases, followed by cases of Transient Tachypnoea of Newborn (TTN) and Respiratory Distress Syndrome (RDS) which were seen in 18 percent and 17 percent cases respectively. Cases of hypoglycemia, asphyxia and IUGR with low birth weight accounted for around 17 percent.
Be a part of Elets Collaborative Initiatives. Join Us for Upcoming Events and explore business opportunities. Like us on Facebook , connect with us on LinkedIn and follow us on Twitter , Instagram.









